The U.S. government is the largest payor of medical costs, through Medicare and Medicaid, and has a strong influence on physician reimbursement. In 2020, Medicare and Medicaid accounted for an estimated $829.5 billion and $671.2 billion in healthcare spending, respectively.1 The prevalence of these public payors in the healthcare marketplace often results in their acting as a price setter, and being used as a benchmark for private reimbursement rates.2
Medicare recently began paying for Remote Therapeutic Monitoring (RTM) through the Medicare Physician Fee Schedule (MPFS). MPFS payments are calculated according to Medicare’s Resource Based Relative Value Scales (RBRVS) system, which is updated annually by the Centers for Medicare & Medicaid Services (CMS). The RBRVS system assigns relative value units (RVUs) to individual procedures based on the resources required to perform each procedure. Under this system, each procedure in the MPFS is assigned RVUs for three categories of resources:
The physician work (wRVU) component, which represents the physician’s contribution of time and effort to the completion of a procedure. The higher the value of the code, the more skill, time, and work it takes to complete;
The practice expense (PE RVU), which is based on direct and indirect physician practice expenses involved in providing healthcare services. Direct expense categories include: clinical labor, medical supplies, and medical equipment. Indirect expenses include: administrative labor, office expenses, and all other expenses; and,
The malpractice (MP RVU) expense, which corresponds to the relative malpractice practice expenses for medical procedures.
3 These values typically comprise the smallest component of the RVU, and due to the variation in malpractice costs among states and specialties, must be weighted geographically and across specialties.
4
Once the procedure’s RVUs have been modified for geographic variance, they are summed, and the total is then multiplied by a conversion factor to obtain the dollar amount of governmental reimbursement for a given service.5
The 2022 MPFS introduced five new general medicine Current Procedural Terminology (CPT) codes for the reimbursement of RTM, effective January 1, 2022:
98975: Remote therapeutic monitoring (e.g., respiratory system status, musculoskeletal system status, therapy adherence, therapy response); initial set-up and patient education on use of equipment.
98976: Remote therapeutic monitoring (e.g., respiratory system status, musculoskeletal system status, therapy adherence, therapy response); device(s) supply with scheduled recording(s) and/or programmed alert(s) transmission to monitor respiratory system, each 30 days.
98977: Remote therapeutic monitoring (e.g., respiratory system status, musculoskeletal system status, therapy adherence, therapy response); device(s) supply with scheduled recording(s) and/or programmed alert(s) transmission to monitor musculoskeletal system, each 30 days.
98980: Remote therapeutic monitoring treatment management services, physician/other qualified healthcare professional time in a calendar month requiring at least one interactive communication with the patient/caregiver during the calendar month; first 20 minutes – base code.
98981: Remote therapeutic monitoring treatment management services, physician/other qualified healthcare professional time in a calendar month requiring at least one interactive communication with the patient/caregiver during the calendar month; each additional add on code 20 minutes (list separately in addition to code for primary procedure).
6
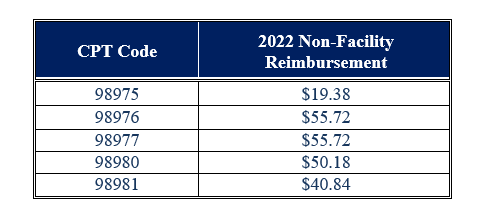
Notably, three of these codes are PE-only codes, while two include professional work (wRVUs). Also of note is that RTM requires the use of a device approved by the U.S. Food & Drug Administration (FDA), and CPT codes 98975, 98976, and 98977 require that device to monitor at least 16 days’ worth of data in each 30-day period.7 The 2022 payment rates for each of these codes are set forth below:8
For 2023, CMS proposes tweaking the RTM codes in response to stakeholder comments and CMS concern regarding who could perform certain codes. CMS suggests discontinuing payment for CPT codes 98980 and 98981; adding four new RTM codes related to monitoring and management services (as HCPCS G codes9); and adding a new CPT code for supplying Cognitive Behavioral Therapy Monitoring (CBTM) devices.
Specifically, CPT codes 98980 and 98981 are proposed to be eliminated and replaced with HCPCS codes GRTM1 and GRTM2,10 which will allow the billing clinician to provide general, rather than direct, supervision, as the requirement to directly supervise staff providing RTM care management services was overburdening billing clinicians.11 The two other new HCPCS codes proposed by CMS (GRTM 3 and GRTM 4) are for assessment services furnished by nonphysician qualified health care professionals (QHCPs) such as physical therapists, occupational therapists, and speech language pathologists.12 Notably, these two codes are designated as “sometimes therapy” codes, which “means that the services could be billed outside a therapy plan of care” if billed by a physician or nonphysician provider, but not if the services are billed by a QHCP.13 The new CPT code for CBTM devices, 989X6, will be a PE-only code “intended to provide reimbursement for RTM devices supplied to patients to monitor a patients’ adherence and response to a prescribed cognitive behavior therapy program.”14 This code is very similar to the device supply CPT codes 98976 and 98977 for respiratory and musculoskeletal devices under the Remote Patient Monitoring (RPM) codes.15
As the 2023 MPFS has not yet been finalized, there are no confirmed updates on the non-facility reimbursement rates for RTM services. Due to the newness of RTM, it is likely that CMS will continue to tweak the coverage of and payment for these services in the years to come through regulatory rulemaking. Consequently, the regulatory environment of RTM will be discussed in the next installment in this series.
“NHE Fact Sheet” Centers for Medicare & Medicaid Services, December 15, 2021, https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NHE-Fact-Sheet (Accessed 8/16/22).
“Physician Panel Prescribes the Fees Paid by Medicare” By Anna Wilde Mathews and Tom McGinty, The Wall Street Journal, October 26, 2010, https://www.wsj.com/articles/SB10001424052748704657304575540440173772102 (Accessed 8/16/22).
“Medicare Program; Payment Policies Under the Physician Fee Schedule and Other Revisions to Part B for CY 2011; Final Rule” Centers for Medicare and Medicaid Services, Federal Register, Vol. 75, No. 228 (November 29, 2010), p. 73208.
Ibid; “Introduction to Relative Value Units and How Medicare Reimbursement is Calculated” American College of Radiation Oncology, http://www.acro.org/washington/RVU.pdf (Accessed 1/13/21); Federal Register, Vol. 75, No. 228 (November 29, 2010).
“Physician Reimbursement Under Medicare” By Alan M. Scarrow, MD, Neurosurgical Focus, Vol. 12, No. 4: Article 8 (April 2002), p. 2.
“Medicare Program; CY 2022 Payment Policies Under the Physician Fee Schedule and Other Changes to Part B Payment Policies; Medicare Shared Savings Program Requirements; Provider Enrollment Regulation Updates; and Provider and Supplier Prepayment and Post-Payment Medical Review Requirements” Federal Register, Vol. 86, No. 221 (November 19, 2021), p. 65114-65117.
“2022 Medicare Remote Therapeutic Monitoring FAQs: CMS Final Rule” By Thomas B. Ferrante, et al., Foley & Lardner LLP, Health Care Law Today, November 11, 2021, https://www.foley.com/en/insights/publications/2021/11/2022-remote-therapeutic-monitoring-cms-final-rule (Accessed 2/15/22).
“2022 Medicare Non-Facility Reimbursement for Care Management Services” Nixon Gwilt Law, available at: https://static1.squarespace.com/static/563c7acce4b028323896cb89/t/61efae41919a2427e0817691/1643097684198/Medicare+Non-Facility+Reimbursement+for+Care+Mgmt+CPT+Codes+2022_NGL.pdf (Accessed 2/16/22).
The Healthcare Common Procedure Coding System (HCPCS) is a set of procedure codes based on the CPT. Temporary G codes are a subset of HCPCS codes assigned to services and procedures that are under review before being included in the CPT coding system.
The acronym GRTM is a combination of the G code indicator and Remote Therapeutic Monitoring (RTM).
“Proposed Changes to Remote Therapeutic Monitoring Reimbursement in the Proposed 2023 Medicare Physician Fee Schedule” Nixon Gwilt Law, July 11, 2022, https://nixongwiltlaw.com/nlg-blog/2022/7/11/proposed-changes-to-remote-therapeutic-monitoring-reimbursement-in-the-proposed-2023-medicare-physician-fee-schedule (Accessed 8/24/22).
“Medicare and Medicaid Programs; CY 2023 Payment Policies Under the Physician Fee Schedule and Other Changes to Part B Payment Policies; Medicare Shared Savings Program Requirements; Medicare and Medicaid Provider Enrollment Policies, Including for Skilled Nursing Facilities; Conditions of Payment for Suppliers of Durable Medicaid Equipment, Prosthetics, Orthotics, and Supplies (DMEPOS); and Implementing Requirements for Manufacturers of Certain Single-Dose Container or Single-Use Package Drugs To Provide Refunds With Respect to Discarded Amounts” Federal Register, Vol. 87, No. 145 (July 29, 2022), p. 46024; Nixon Gwilt Law, July 11, 2022.
Federal Register, Vol. 87, No. 145 (July 29, 2022), p. 46024.
Nixon Gwilt Law, July 11, 2022.
For more information on the difference between RTM and RPM, see “Valuation of Remote Therapeutic Monitoring: Introduction” Health Capital Topics, Vol. 15, Issue 7 (July 2022), https://www.healthcapital.com/hcc/newsletter/07_22/HTML/RTM/convert_valuation-of-rtm---overview-7.26.22.php (Accessed 8/24/22); “Proposed Changes to Remote Therapeutic Monitoring Reimbursement in the Proposed 2023 Medicare Physician Fee Schedule” Nixon Gwilt Law, July 11, 2022, https://nixongwiltlaw.com/nlg-blog/2022/7/11/proposed-changes-to-remote-therapeutic-monitoring-reimbursement-in-the-proposed-2023-medicare-physician-fee-schedule (Accessed 8/24/22).






