Home health agencies (HHAs) are primarily engaged in providing “a wide range of health care services that can be given in [a] home for an illness or injury.”1 There are three types of services that typically fall under the umbrella of home healthcare: (1) home healthcare enterprises, which provide medical and supportive care; (2) home care aide enterprises, which provide nonmedical care or custodial/non-meal care; and (3) hospice enterprises, which provide end-of-life care.2 Additionally, two of the main types of home healthcare services are: (1) infusion therapy and (2) respiratory therapy.3 Utilization of home healthcare services “rises with the number of chronic conditions and the functional impairments that people have,” with approximately two-thirds of all Medicare home healthcare users managing at least four chronic conditions and at least one functional impairment.4 While the elderly are frequent recipients of home healthcare services, chronically ill persons of all ages may also utilize home healthcare services.5
Lawmakers and regulators have historically viewed home health services with apprehension, largely due to the high potential for fraud and abuse.6 These concerns have led to Medicare payment cuts and new regulatory hurdles for home health providers at a time when home healthcare is becoming more popular with the elderly population.7 Further complicating the healthcare landscape, approximately 10,000 Baby Boomers will reach retirement age every day through 2030,8 which will affect how policy makers and healthcare providers shape the healthcare delivery system.9 As these Baby Boomers retire, not only may it increase demand for home healthcare services, but it may also decrease the supply of healthcare providers, as a number of HHAs are simply ceasing operations when their owners retire, and home care workers (also known as direct care workers) are difficult to recruit due to the profession’s low pay, inconsistent schedule, and lack of advancement opportunities.10 As the Baby Boomer generation retires, competition between HHAs, skilled nursing facilities (SNFs), and hospital outpatient facilities may increase due to an increasing patient pool.11 However, given the growing interest in home health utilization among the elderly population, due to its cost-effective means of delivering care while allowing them to stay in their homes, the future of home health may be bright for providers able to leverage finite resources to advance high value care.12
A growing number of elderly persons seeking skilled care are finding value in receiving care at home. Individuals age 45+ have exhibited strong preference for independent living in their homes versus other alternatives.13 Patient-centered care, as defined by the Institute of Medicine, is “providing care that is respectful of and responsive to individual patient preferences, needs, and values and ensuring that patient values guide all clinical decisions.”14 For many patients, receiving treatment in their home allows the care to be tailored to their specific needs,15 including being individualized to their home settings, daily behaviors, and specialized needs, which can improve quality of care and patient satisfaction.16
The aging Baby Boomers population, coupled with increased utilization of healthcare services (given that this population segment has higher rates of diabetes and obesity than their parents),17 will likely increase the patient pool for healthcare services relating to chronic disease management. Two-thirds (66%) of Medicare beneficiaries suffer from at least two chronic conditions, and of that portion, 15% suffer from six or more chronic conditions;18 the most common conditions among Medicare beneficiaries, as of 2018, are represented in the below exhibit.
Exhibit: Percentage of Medicare Fee-For-Service (FFS) Beneficiaries with Chronic Conditions, 201819
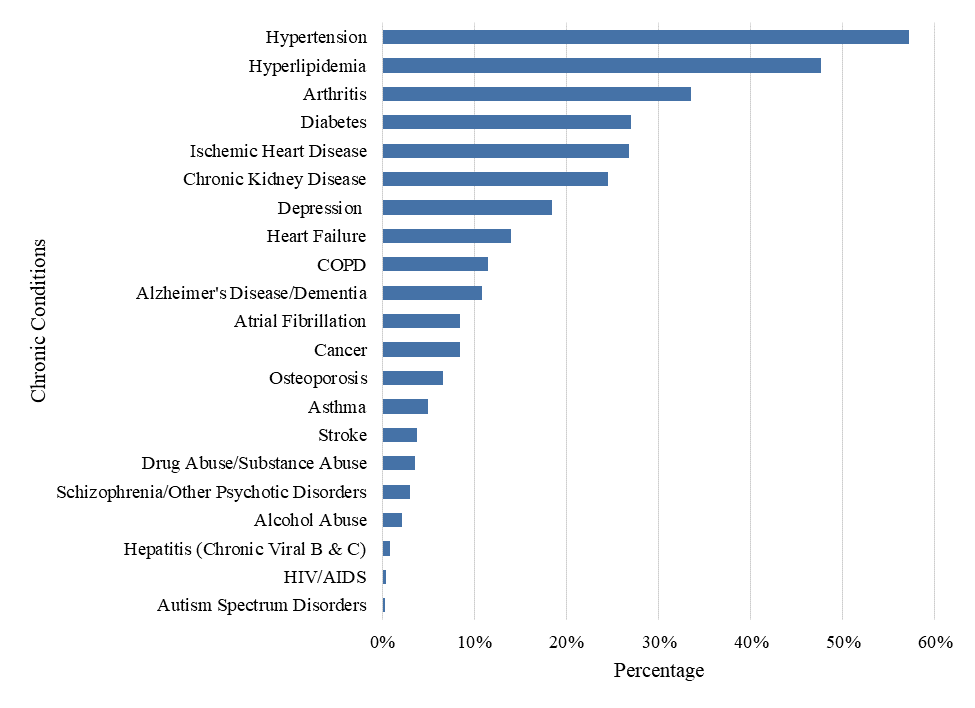
Patients with chronic conditions under the age of 65 have also become strong advocates for receiving care in their home. Chronic diseases are among the most prevalent health problems in the U.S., with approximately 60% of the U.S. population having at least one chronic condition, and approximately 40% having multiple chronic conditions (predictably, the prevalence of multiple chronic conditions are highest in older adults).20 Seven out of ten deaths among Americans every year result from chronic diseases, including: (1) heart disease; (2) cancer; and, (3) diabetes.21
Patient preference for home health is being increasingly matched by payors, who have recognized the cost effectiveness of home healthcare. As national healthcare expenditures per capita continue to rise,22 a shift toward cost effective healthcare delivery may be imminent. In 2019, the average cost for an in-home health visit was $13,012, which was roughly $7,000 less than the same visit at an in-patient facility ($20,325).23 Extrapolating home health services nationwide for just five conditions could result in $3.7 billion in overall cost savings and $3 billion in Medicare savings.24 Further, home healthcare represents 13% of all Medicare episodes utilizing post-acute care after hospital discharge.25 While not as costly as skilled nursing facilities (SNFs), inpatient rehabilitation facilities (IRFs), or long-term acute care hospitals (LTCHs), 84% of Medicare home health patients rate their overall care a “9” or “10” on a ten-point scale.26 Additionally, 92% of home health patients receiving wound care noted improvement or healing after an operation, 82% bathed more easily after a home health regimen, and 83% of home health patients noted improved breathing after a home health regimen.27
As the healthcare system evolves and is reformed to meet the future needs of the rapidly aging U.S. population, the value of healthcare delivery at home may grow due to patients’ familiarity with technology, their preference to be treated at home, and home health’s cost effective means of delivering high-quality care. However, with the continuing intense regulatory scrutiny of these healthcare organizations, HHAs should be cognizant of the potential for over-utilization of home health services that may subject them to fraud and abuse inquiry. The second installment of this five-part series will therefore cover the regulatory environment in which home health agencies operate.
“What’s Home Health Care & What Should I Expect?” Medicare.gov, https://www.medicare.gov/what-medicare-covers/whats-home-health-care (Accessed 1/20/22).
“IBISWorld Industry Report 62161: Home Care Providers in the US” By Dmitry Diment, IBIS World, August 2021, p. 5, 19.
“The Future of Home Health Care: Workshop Summary, Institute of Medicine, Washington, D.C.: National Academy of Sciences, 2015, p. 37.
“OIG Online Portfolio: Home Health” Office of Inspector General, February 9, 2016, https://oig.hhs.gov/reports-and-publications/portfolio/home-health/ (Accessed 1/20/22).
“The Future of Home Health Care: A Strategic Framework for Optimizing Value” Steven Landers, et al., Home Health Care Management & Practice, Vol. 28, No. 4 (2016), available at: https://journals.sagepub.com/doi/pdf/10.1177/1084822316666368 (Accessed 1/20/22), p. 264-265, 267; “CMS proposes chopping $1 billion from home health reimbursement over two years” By Virgil Dickson, Modern Healthcare, July 25, 2017, https://www.modernhealthcare.com/article/20170725/NEWS/170729937/cms-proposes-chopping-1-billion-from-home-health-reimbursement-over-two-years (Accessed 1/20/22).
“Baby Boomers Approach 65 – Glumly” By D’Vera Cohn and Paul Taylor, Pew Research Center, December 20, 2010, http://www.pewsocialtrends.org/2010/12/20/baby-boomers-approach-65-glumly/ (Accessed 1/120/22).
Landers, et al., Home Health Care Management & Practice, Vol. 28, No. 4 (2016), p. 262-278.
“The Shortage Of Home Care Workers: Worse Than You Think” By Chris Farrell, Forbes, April 18, 2018, https://www.forbes.com/sites/nextavenue/2018/04/18/the-shortage-of-home-care-workers-worse-than-you-think/#34f88f1e3ddd (Accessed 1/20/22).
Institute of Medicine, Washington, D.C.: National Academy of Sciences, 2015, p. 60.
“The Future of Home Health Care Project” The Alliance for Home Health Quality & Innovation, May 2014, http://www.ahhqi.org/images/pdf/future-whitepaper.pdf (Accessed 1/20/22), p. 5, 12.
Landers, et al., Home Health Care Management & Practice, Vol. 28, No. 4 (2016), p. 262-278.
“Crossing the Quality Chasm: A New Health System for the 21st Century” Institute of Medicine, Executive Summary, March 2001, p. 29, https://www.ncbi.nlm.nih.gov/books/NBK222274/pdf/Bookshelf_NBK222274.pdf (Accessed 1/21/22).
The Alliance for Home Health Quality & Innovation, May 2014, p. 7-8.
“Patient-Centered Care: What It Means And How To Get There” By James Rickert, Health Affairs Blog, January 24, 2012, http://healthaffairs.org/blog/2012/01/24/patient-centered-care-what-it-means-and-how-to-get-there/ (Accessed 1/21/22).
“America’s Health Rankings” United Health Foundation, 2021, available at: https://assets.americashealthrankings.org/app/uploads/americashealthrankings-2021annualreport.pdf (Accessed 1/20/22).
“Datatables_for_chronic_conditions_charts_2018.xlxs” from “Charts and Chartbooks” Centers for Medicare & Medicaid Services, available at: https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Chronic-Conditions/Chartbook_Charts (Accessed 1/21/22).
“Figure 1: Prevalence of Chronic Conditions among Fee-for-Service Beneficiaries: 2018” Centers for Medicare & Medicaid Services, available at: https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/Chronic-Conditions/Chartbook_Charts (Accessed 1/21/22).
“Chronic Diseases in America” CDC’s National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP), https://www.cdc.gov/chronicdisease/pdf/infographics/chronic-disease-H.pdf (Accessed 1/20/22); “Multiple Chronic Conditions in the United States” By Christine Buttorff, et al., RAND Corporation, 2017 http://www.fightchronicdisease.org/sites/default/files/TL221_final.pdf (Accessed 1/20/22), p. 25.
“The Growing Crisis of Chronic Disease in the United States” Partnership to Fight Chronic Disease, https://www.fightchronicdisease.org/sites/default/files/docs/GrowingCrisisofChronicDiseaseintheUSfactsheet_81009.pdf (Accessed 1/20/22).
“National Health Expenditures -- Projections 1960-2028” Centers for Medicare and Medicaid Services, March 3, 2020, https://www.cms.gov/research-statistics-data-and-systems/statistics-trends-and-reports/nationalhealthexpenddata/nationalhealthaccountsprojected (Accessed 1/21/22).
“New Study Shows Home Health More Effective than Hospital Stay for Many Patients” Partnership for Quality Home Healthcare, March 19, 2019, https://pqhh.org/new-study-shows-home-health-more-effective-than-hospital-stay-for-many-patients/#:~:text=March%2019%2C%202019-,New%20Study%20Shows%20Home%20Health%20More%20Effective%20than%20Hospital%20Stay,provide%20to%20patients%20every%20day.&text=In%20other%20words%2C%20research%20suggests,win%20for%20patients%20and%20Medicare. (Accessed 2/16/22).
“Improved Cost and Utilization Among Medicare Beneficiaries Dispositioned From the ED to Receive Home Health Care Compared With Inpatient Hospitalization” By James Howard, MD, et al., The American Journal of Accountable Care, March 4, 2019, https://www.westhealth.org/resource/the-american-journal-of-accountable-care-improved-cost-and-utilization-among-medicare-beneficiaries-dispositioned-from-the-ed-to-receive-home-health-care-compared-with-inpatient-hospitalization/ (Accessed 1/21/22).
“Home Health Chartbook 2021: Prepared for the Alliance for Home Health Quality and Innovation (AHHQI)” Alliance for Home Health Quality and Innovation, September 2021, https://ahhqi.org/images/uploads/AHHQI_2021_Home_Health_Chartbook_FINAL.pdf (Accessed 1/21/22), p. 40.
The Alliance for Home Health Quality & Innovation, May 2014, p. 5.
“Table 6.7: National Averages for Patient Outcomes while in Home Health Care, 2020” in “Home Health Chartbook 2021: Prepared for the Alliance for Home Health Quality and Innovation” Avalere Health, September 2021, https://ahhqi.org/images/uploads/AHHQI_2021_Home_Health_Chartbook_FINAL.pdf (Accessed 1/21/22), p. 66.






